Preterm birth (PTB) is a global health crisis, affecting 15 million babies every year and contributing to over 1 million child deaths annually. Despite advances in neonatal care, the root cause of many early deliveries—inflammation in gestational tissues—remains poorly addressed by current treatments. But a groundbreaking 2025 study published in EMBO Molecular Medicine has introduced a game-changing therapeutic: HSJ633, a small peptide that selectively targets the IL-6 receptor (IL-6R) to prevent PTB and protect newborn health.
Why Current Treatments Fall Short
Current therapies like tocolytics only suppress uterine contractions. They do not target inflammation, leaving fetuses exposed to harmful cytokines that damage developing organs like the lungs, intestines, and brain.
One cytokine in particular, interleukin-6 (IL-6), plays a central role in initiating inflammation-induced labor. IL-6 levels surge in the amniotic fluid during infection, making it a prime target. Unfortunately, existing drugs like Tocilizumab, which block IL-6 signaling completely, also disrupt protective signaling pathways needed by the fetus—posing risks of immunosuppression and developmental harm.
Enter HSJ633: The First Biased Allosteric IL-6R Modulator
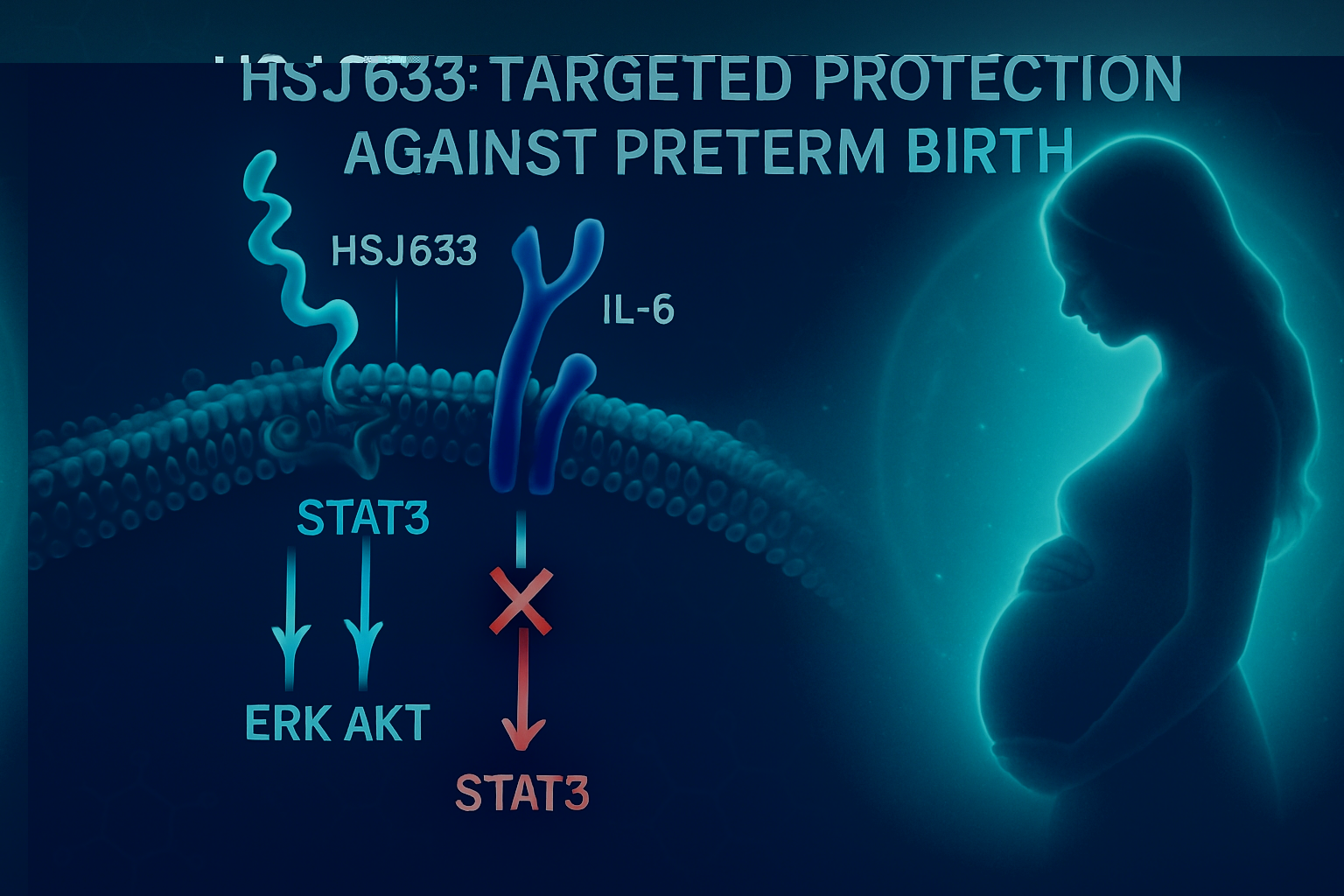
Researchers have now designed HSJ633, a small 9-amino-acid peptide that binds to the IL-6 receptor at a unique allosteric site, away from the typical IL-6 binding region.
Unlike monoclonal antibodies, HSJ633 doesn’t shut down the entire signaling cascade. Instead, it selectively blocks STAT3—a key driver of inflammatory gene expression—while preserving ERK, AKT, and p38 pathways, which are critical for cell survival and fetal development.
This “biased signaling” strategy offers therapeutic precision previously unseen in anti-inflammatory treatments during pregnancy.
What the Mouse Models Showed
In a well-established mouse model of PTB triggered by lipopolysaccharide (LPS)—a bacterial toxin mimicking infection—HSJ633 showed remarkable effects:
- Reduced inflammation in uterus, placenta, and fetal membranes
- Lowered preterm birth rate from 93% to 22%
- Increased neonatal survival from 33% to 87%
- Preserved lung and intestinal structure in pups
- Increased birth weight and organ development
Even more impressive, HSJ633 worked both prophylactically and therapeutically. Administered 2 hours after inflammation began, it still improved outcomes—mirroring a potential 30-hour window in human gestation.
Effective in Human Tissues Too
To bridge the gap to clinical relevance, the researchers tested HSJ633 on human fetal membrane explants from term pregnancies. When stimulated with HMGB1, a molecule that induces sterile inflammation, tissues showed a dramatic reduction in IL-1β and IL-6 after HSJ633 treatment.
This ex vivo success shows HSJ633’s cross-species efficacy, validating its therapeutic potential for human use.
A Safer Alternative to Current IL-6R Drugs
Unlike monoclonal antibodies that indiscriminately block all IL-6 signaling, HSJ633:
- Does not interfere with protective cytokine pathways
- Preserves fetal immune development
- Shows better safety profile for pregnant women
- Selectively targets the soluble IL-6R, the main driver of inflammation during PTB
In essence, HSJ633 decouples inflammation from fetal protection, offering a tailored solution for maternal-fetal medicine.
The Science Behind the Selectivity
HSJ633 works by binding to IL-6R at a remote site, changing the receptor’s shape in a way that prevents STAT3 phosphorylation—a crucial step in inflammation. Meanwhile, it leaves ERK, p38, and AKT untouched, helping tissues grow and repair normally.
The study also confirmed that blocking STAT3 alone, using a separate compound, was enough to prevent preterm birth in mice. This supports the idea that STAT3 is the key switch, and HSJ633 is the most precise tool yet to flip it.
What This Means for the Future
This breakthrough sets the stage for a new era in preterm birth prevention. With its biased, allosteric mechanism, HSJ633 may:
- Delay labor without harming fetal development
- Provide a 30+ hour therapeutic window
- Work in infection and sterile inflammation models
- Lead to next-generation anti-inflammatory drugs for obstetrics
If clinical trials confirm safety and efficacy in humans, HSJ633 could become the first therapy to truly prevent inflammation-induced preterm birth—saving millions of babies from a lifetime of complications.
Check out the cool NewsWade YouTube video about this article!
Article derived from: Côté, F., Prairie, E., Sierra, E. M., Quiniou, C., Habelrih, T., Xu, W., Ferri, B., Hou, X., Lahaie, I., Côté, N., Loiselle, S., Gobeil, L., Sawaya, K., Faucher, A., Beaulieu, A., Delisle, S., Simard, M., Nezhady, M. a. M., Laplante, V., . . . Chemtob, S. (2025). A novel modulator of IL-6R prevents inflammation-induced preterm birth and improves newborn outcome. EMBO Molecular Medicine. https://doi.org/10.1038/s44321-025-00257-9